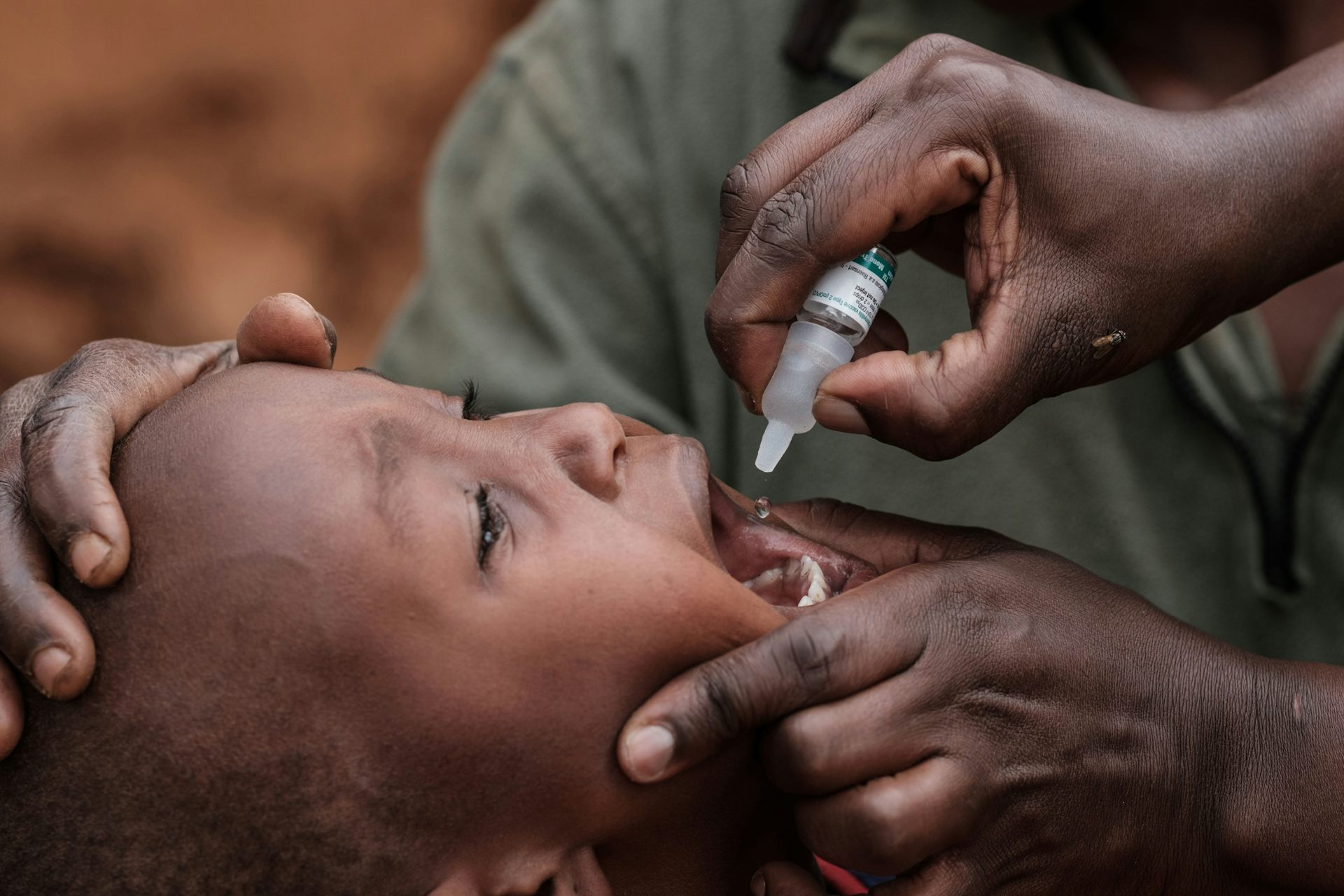
Polio was one of the most dreaded diseases in the world in the 20th century. Four decades ago, an estimated 350,000 people were paralysed each year by the poliovirus in more than 125 countries. This led the World Health Assembly in 1988 to adopt a resolution for the worldwide eradication of polio, drawing inspiration from the eradication of smallpox.
The global programme to eradicate polio is spearheaded by a number of actors. These include national governments, the World Health Organisation (WHO), multiple development agencies, and healthcare workers.
The strategy involves widespread vaccination as part of routine healthcare services as well as mass vaccination campaigns. Sensitive surveillance to detect and rapidly respond to polio cases is also key.
This initiative has been extremely successful. The number of people paralysed by polio decreased by 99.9% – from 350,000 in 1988 to 175 in 2019. During the same period, the number of polio endemic countries fell from more than 125 to only two: Afghanistan and Pakistan. A country is endemic when there’s widespread circulation of polio.
The latest WHO region to be certified polio free is Africa. The region was certified on 25 August 2020. The certification came four years after the last case of poliovirus on the continent.
The polio eradication programme in Africa directly combated a severe debilitating disease. But it also provided a platform for broader healthcare services on the continent. Polio eradication created renewed demand for vaccination services and innovative ways to deliver healthcare services.
What does it take to eradicate a disease?
It takes a combination of multiple biological and non-biological factors to eradicate a disease. Only one disease, smallpox, has so far been eradicated.
Polio viruses only survive for a very short time in the environment and there are no animal or insect reservoirs that carry polio viruses. More importantly, effective vaccines exist against polio. Beyond these biological features of polio, the eradication of polio from Africa required sound leadership.
In 1996 African heads of state resolved to stamp polio out of Africa. Then South African President Nelson Mandela launched the “Kick Polio out of Africa” campaign. Thereafter, all-of-society collaborations supporting widespread polio vaccination sprang up across African countries. These involved government departments, the private sector, the civil society, and the community at large to ensure eradication of polio from the continent.
Within national governments in Africa, public service departments worked across portfolio boundaries, formally and informally, to achieve the shared goal of polio eradication. All these efforts culminated, 14 years later, in the certification of the eradication of polio from Africa.
Certification is based on evidence that something has been achieved. In the case of polio eradication, a region only gets certified when all the countries in the area demonstrate the absence of poliovirus transmission for at least three consecutive years in the presence of extremely sensitive surveillance.
Polio surveillance refers to a disease detection system that involves both community and laboratory components.
Surveillance in the community is done by the general public and healthcare workers. Healthcare workers need to report all cases of children who experience abrupt weakness of the limbs. Community members need to report any newly paralysed children in their communities to healthcare services. In the laboratory, the polio virus responsible for any case of polio paralysis is identified and its source determined. Without such high-quality surveillance it would be difficult to locate where and exactly how the polio virus is circulating or to confirm when its transmission has been eradicated.
Twenty years ago, Africa was close to polio eradication; then misinformation surfaced in northern Nigeria about the effectiveness and safety of polio vaccines. This misinformation led some people in the area to refuse or delay polio vaccines. Vaccination coverage dropped, resulting in widespread polio outbreaks in northern Nigeria and beyond. Such misinformation has gained traction on social media.
Avoiding vaccination even when it’s available is referred to as vaccine hesitancy. Polio vaccine hesitancy poses significant risks not only for the hesitant people, but also the wider community. It could prevent African communities from reaching thresholds of vaccination coverage necessary to keep polio out of Africa. If a single child remains infected with polio virus in any part of the world, children in all countries are at risk of contracting the disease.
Long-term rewards
Africa’s health systems are much stronger because of the investments made. Countries were supported to make life-saving gains. These included increasing access to health care in the most remote places, strengthening routine vaccination systems, and ensuring strong disease surveillance.
Polio’s legacy must be built on to achieve other major health goals.![]()
Charles Shey Wiysonge, Director, Cochrane South Africa, South African Medical Research Council
This article is republished from The Conversation under a Creative Commons license.

